Past Programs at One Mind: AURORA

AURORA is an unprecedented national research initiative working to improve the understanding, resilience, and recovery of individuals who have experienced a traumatic event.
About AURORA
Post-traumatic stress (PTS) and related adverse psychiatric outcomes such as depression, anxiety and pain, are common in the millions of Americans who experience traumatic events, such as motor vehicle collisions, sexual assault, adverse childhood events, and the severe illness or death of others. An estimated 8% of Americans – 24.4 million people – live with PTS, impairing daily function and frequently causing long-term disability.
In the wake of COVID-19, the volume and rates of PTS diagnosis have dramatically risen. Key groups experiencing a higher burden of PTS and related adverse psychiatric outcomes from current epidemics of trauma include healthcare workers, marginalized communities suffering discrimination, and veterans. Sadly, the existing methods of diagnosing PTS, as well as the understanding of the biological underpinnings that cause the illness, remain limited.
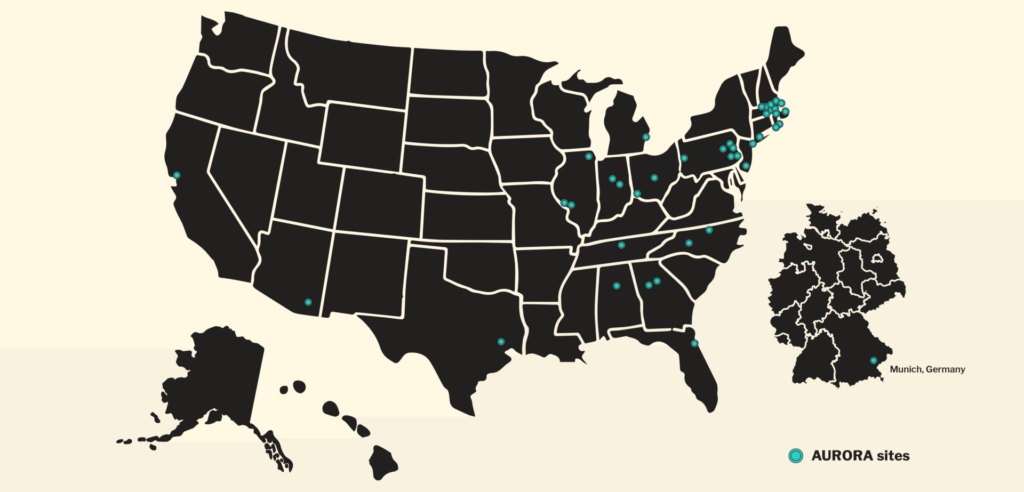
In September 2016, the National Institute of Mental Health put forth $21 million to support and launch the AURORA study. Led by scientists at the University of North Carolina and Harvard and supported by 17 other institutions, AURORA is applying the latest tools in physiology, genomics, neuroimaging, and wearable technology to achieve a quantum leap in knowledge that trauma survivors so desperately need. Enrolling its first study participant in September 2017, AURORA intends to collect and analyze data from 5,000 trauma patients during a 5-year period, enrolling study participants at 30 emergency department recruitment sites located throughout the United States. As a result, AURORA will be the largest, most comprehensive trauma study ever performed.
Although the NIMH funding provides tremendous support for AURORA, significant gaps in the original financing prevent the participating investigators from fully exploiting and accelerating the opportunity this large cohort of patients represents. In order to accelerate the outcomes of the AURORA study, in 2017 One Mind set out to raise an additional $6.8 million in donor-generated funds. As of November 2022, One Mind has given $6 million to AURORA.
Recent News: Feelings of Detachment Predict Worse Mental Health Outcomes After Trauma
Goals
- Deliver tools for clinicians to make informed decisions about trauma survivors’ risk and care
- Identify new intervention targets that will give rise to personalized, precision treatments for neuropsychiatric trauma
Making An Impact For Trauma Survivors
AURORA has already enrolled almost 3,500 participants. Researchers are collecting patients’ blood samples, obtaining real time data through the patient’s Verily Study Watch (donated from Google), and performing MRIs. The study identifies multidimensional outcomes of a traumatic event the way that patients actually experience symptoms— not one at a time, but in combination with each other. Once identified, each outcome is simultaneously studied in real time and tracked over an extended period, resulting in a detailed biological and behavioral assessment. This level of depth has never been undertaken before when studying symptoms following trauma.
AURORA is generating an unprecedented data library for researchers around the globe to use, which will catalyze new understanding and treatments in the field of trauma interventions. Early results have been extremely promising, fueling many new discoveries like potential preventative treatments. The AURORA researchers have identified and initiated validation studies on over 200 biomarkers, remarkable and unprecedented progress.
Partners
AURORA is a collaborative effort between 40 leading scientists from 19 institutions that include Harvard and UNC- Chapel Hill, the two institutions that spearheaded the study. AURORA was launched with an initial financial commitment from the NIMH, the Department of Defense, and One Mind.
