TRACK-TBI Researchers Identify Risk Factors for the Development of Neuropsychiatric Conditions after Concussion:
Researchers in the One Mind-supported Transforming Research and Clinical Knowledge in Traumatic Brain Injury (TRACK-TBI) Initiative have identified risk factors for the development of neuropsychiatric conditions after concussion. As published this week in JAMA Psychiatry, University of California San Diego’s Murray B. Stein, M.D., MPH and his colleagues found that for those who sustain a mild traumatic brain injury (mTBI), also known as a concussion, approximately 1 in 5 experience mental health symptoms up to 6 months after their mTBI.
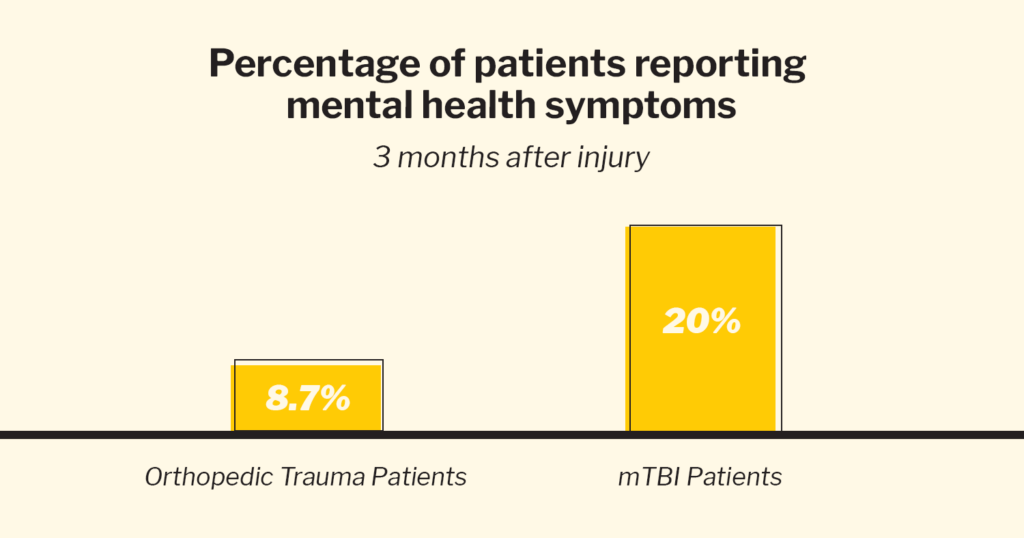
By investigating the mental health outcomes of 1,155 people who had experienced a mild TBI and were treated in an emergency department, Dr. Stein and his team found that at 3 months after their initial visit, 20 percent of the mTBI patients reported mental health symptoms such as Post-Traumatic Stress or Major Depressive Disorder, while only 8.7 percent of patients who sustained an orthopedic trauma, such as a broken limb, reported such symptoms. And after 6months, 21.2 percent of the mTBI patients reported mental health symptoms, compared to 12.1 percent of the orthopedic trauma patients. These findings support prior research done by TRACK-TBI that was published in JAMA Network Open in May 2018 (that One Mind wrote about) that highlights the need for better follow-up care after an mTBI patient’s initial emergency department visit.
Additionally, Dr. Stein and his team used the TRACK-TBI data to research possible risk factors for PTS and major depressive disorder after experiencing an mTBI. Lower levels of education, having a history of mental illness and self-identifying as an African American were all shown to increase the risk. In addition, if the head injury was caused by an assault or other violent attack, the risk of developing post-traumatic stress increased.
As stated in the National Institutes of Health’s press release highlighting this study, Dr. Stein states “Contrary to common assumptions, mild head injuries can cause long-term effects. These findings suggest that follow-up care after head injury, even for mild cases, is crucial, especially for patients showing risk factors for PTSD or depression”.
In addition to providing financial support to the TRACK-TBI Initiative, One Mind also intends to raise $7.9 million ($2 million donated to date) for the AURORA study, launched in 2016, that aims to deliver clinical decision tools, biomarkers and new treatments to patients who develop post-traumatic stress, depression and pain after experiencing a traumatic event. As part of our initial support of the AURORA study, One Mind provided the impetus and know-how to AURORA to ensure that the data from their study was and continues to be collected and formatted using the same NIH/NINDS Common Data Elements as TRACK-TBI. In understanding the immense value that transdiagnostic data sharing provides, One Mind remains steadfast in supporting the TRACK-TBI and AURORA studies to harmonize their data to create a first-of-its-kind ‘collaboratory’ dataset that could be leveraged to accelerate the research of the comorbidity of these brain health conditions.
Learn more about our support of both of these studies and how you can help here:
